Pharmacy Benefits Management (PBM) Services
Making Medication Access Easier to Navigate
Simplifying complexity across PBM operations while reducing friction throughout the medication access journey
Transform your customer experience
Discover how Everise delivers confidence through innovative, empathetic CX solutions that drive business growth.
Challenges
Simplifying complexity across PBM operations
PBMs face growing operational complexity, volatile demand, margin pressure, and fragmented member experiences. Everise helps PBMs stabilize service delivery, scale efficiently, and maintain compliance with specialized talent and intelligent workflows.
01
Regulatory and Market Disruption
Regulatory and Market Disruption
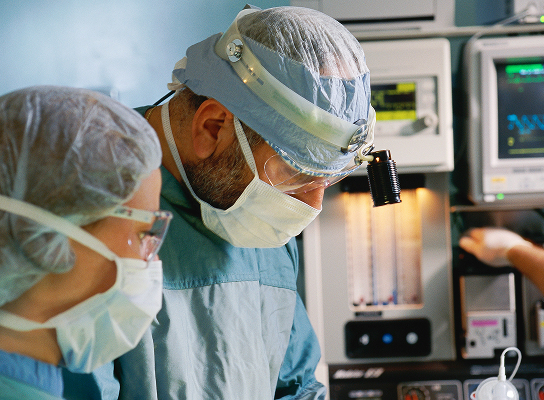
Federal and state reforms, including rebate transparency requirements and Medicare Part D compensation changes, are reshaping PBM operating models. These shifts increase compliance pressure, compress margins, and create confusion for members and providers, driving higher service demand and operational strain.
02
Fluctuating service demand
Fluctuating service demand
Enrollment cycles, benefit changes, and shifts in medication utilization create sharp and often unpredictable volume fluctuations across PBM operations. Fixed staffing models struggle to flex with demand, leading to delays, inconsistent service levels, and access disruptions during peak periods.

03
Shrinking margins
Shrinking margins
Market transparency requirements, rebate model changes, and rising medication costs are compressing PBM margins while service demands continue to grow. Without cost flexibility, PBMs face increasing pressure to sustain profitability while still meeting performance, compliance, and experience expectations.

04
Fragmented member experiences
Fragmented member experiences
Frequent changes across plans, processes, and access pathways have fragmented the member experience, creating confusion and inconsistency at critical moments of care. When access is difficult to navigate, adherence declines, support costs rise, and trust and health outcomes are put at risk.

Impact
PBM operations at scale
Everise supports leading U.S. PBMs through global, industry-trained talent and intelligent solutions, simplifying non-clinical operational complexity and delivering consistent, reliable member experiences.
Significant market presence
of the Top 5 U.S. PBMs supported
Global PBM delivery
PBM-trained champions across 7 global locations
Trusted member experience
Net promoter score
Approach
Seamless Prescription Journey
We support members, providers, and pharmacies throughout the prescription journey by coordinating prior authorization intake and follow-up, coverage determinations and appeals, specialty onboarding, refill coordination, and pharmacy helpdesk workflows. This reduces friction across systems and stakeholders, accelerates medication starts, and helps ensure timely, reliable access to therapy
Member & provider support
High-touch inbound and outbound support for coverage questions, prior authorization status, appeals, and access issues delivered in alignment with Medicare Part D and CMS documentation standards, maintaining audit-ready workflows while reducing provider callbacks and improving member confidence
Utilization & access support
Support across prior authorization intake and follow-up, utilization management workflows, refill coordination, and adherence outreach designed to minimize delays, prevent pharmacy abandonment, and support appropriate medication use while meeting regulatory and clinical requirements
Pharmacy & claims support
Transform your customer experience
Discover how Everise delivers confidence through innovative, empathetic CX solutions that drive business growth.
Insights
The Latest in Pharmacy Benefits Management
Expert perspectives on trends, innovation, and transformation in PBM customer experience.







